Ophthalmic profile and systemic features of pediatric facial nerve palsy
阅读量:987
DOI:doi: 10.3978/ j.issn.1000-4432.2015.11.16
发布日期:2025-01-01
作者:
Preeti Patil-Chhablani
展开更多 '%20fill='white'%20fill-opacity='0.01'/%3e%3cmask%20id='mask0_3477_29692'%20style='mask-type:luminance'%20maskUnits='userSpaceOnUse'%20x='0'%20y='0'%20width='16'%20height='16'%3e%3crect%20id='&%23232;&%23146;&%23153;&%23231;&%23137;&%23136;_2'%20x='16'%20width='16'%20height='16'%20transform='rotate(90%2016%200)'%20fill='white'/%3e%3c/mask%3e%3cg%20mask='url(%23mask0_3477_29692)'%3e%3cpath%20id='&%23232;&%23183;&%23175;&%23229;&%23190;&%23132;'%20d='M14%205L8%2011L2%205'%20stroke='%23333333'%20stroke-width='1.5'%20stroke-linecap='round'%20stroke-linejoin='round'/%3e%3c/g%3e%3c/g%3e%3c/svg%3e)
关键词
Facial nerve palsy (FNP)
amblyopia
neuroimaging
摘要
Background: Facial nerve palsy (FNP) occurs less frequently in children as compared to adults but most
cases are secondary to an identifi able cause. These children may have a variety of ocular and systemic features
associated with the palsy and need detailed ophthalmic and systemic evaluation.
Methods: This was a retrospective chart review of all the cases of FNP below the age of 16 years, presenting
to a tertiary ophthalmic hospital over the period of 9 years, from January 2000 to December 2008.
Results: A total of 22 patients were included in the study. The average age at presentation was 6.08 years
(range, 4 months to 16 years). Only one patient (4.54%) had bilateral FNP and 21 cases (95.45%) had
unilateral FNP. Seventeen patients (77.27%) had congenital palsy and of these, fi ve patients had a syndromic
association, three had birth trauma and nine patients had idiopathic palsy. Five patients (22.72%) had an
acquired palsy, of these, two had a traumatic cause and one patient each had neoplastic origin of the palsy,
iatrogenic palsy after surgery for hemangioma and idiopathic palsy. Three patients had ipsilateral sixth
nerve palsy, two children were diagnosed to have Moebius syndrome, one child had an ipsilateral Duane’s
syndrome with ipsilateral hearing loss. Corneal involvement was seen in eight patients (36.36%). Amblyopia
was seen in ten patients (45.45%). Neuroimaging studies showed evidence of trauma, posterior fossa cysts,
pontine gliosis and neoplasms such as a chloroma. Systemic associations included hemifacial macrosomia,
oculovertebral malformations, Dandy Walker syndrome, Moebius syndrome and cerebral palsy.
Conclusions: FNP in children can have a number of underlying causes, some of which may be life
threatening. It can also result in serious ocular complications including corneal perforation and severe
amblyopia. These children require a multifaceted approach to their care.
全文
Introduction
Facial nerve palsy (FNP) occurs less frequently in children
as compared to adults(1), but maybe a major cause of ocular
morbidity. While most facial nerve palsies in adults are
idiopathic, a secondary cause is present in 70% of pediatric
cases(2). These cases require detailed ophthalmologic and
systemic evaluation. FNP in children may have congenital
or acquired etiology(3). These children may have additional
ocular and systemic features and may require medical care.
The ophthalmologist may be the first point of care
for children with FNP, especially those with associated ocular motility deficits or lid abnormalities. It is thus
important that the pediatric ophthalmologists are aware
of the potential associations of FNP and are tuned to the
needs of these children. Management of pediatric FNP
requires a multifaceted approach including pediatricians,
otorhinolaryngologists, neurologists and ophthalmologists.
There have been no major studies on the ophthalmic
manifestations of pediatric FNP, to the best of our
k nowledge. This study looks at the various ocular
manifestations and systemic associations in 22 children
presenting with FNP and their response to various
treatment modalities.
The other systemic associations included cleft lip and palate, developmental delay and cerebral palsy.
Imaging studies were available in nine patients (40.90%). Of these, two patients had history of trauma with both the CT scans showing fracture of the occipital bone along with the petrous part of the temporal bone. One patient had an MRI scan showing a posterior fossa cyst and was diagnosed as Dandy Walker syndrome. In another patient, with ipsilateral sixth nerve palsy, MRI scan was suggestive of focal atrophic gliosis in the pons. Another patient, showed an intracranial lesion suggestive of a chloroma. One patient, with Moebius syndrome, showed a thinning of the lateral rectus muscle with absent parotid gland and temporalis muscle on computed tomography (CT) scan. One patient with HFM showed small middle ear cavity with ossicular chain deformity on CT scan. Two patients had normal imaging studies.
Materials and methods
This was a retrospective study that included all children
(under the age of 16 years) presenting for an ocular
examination to a tertiary eye center in South India, who
were diagnosed to have FNP, over the period of 1 year.
Institutional Review Board (IRB)/Ethics Committee
decided approval was not required for this study.
A detailed analysis of all the records, with respect to the ocular findings, systemic diagnoses, neuroimaging fi ndings and response to management modalities was done. All the children underwent a complete assessment, including medical history and ophthalmological and orthoptic examinations. An experienced pediatric ophthalmologist evaluated them and the neuroimaging studies, where available, were reviewed by a neuroradiologist. Visual acuity was recorded with the help of a Snellen’s chart and in cases where verbal visual acuity measurements were not possible due to age or associated systemic issues, the testing of visual response was done by monitoring the fixation in each eye by the Central, Steady, Maintained (CSM) method, where C refers to centrality and can be assessed by the location of the corneal light reflex as the patient looks at the examiner’s light with the opposite eye occluded, S refers to the steadiness of fixation on the examiner’s light under monocular conditions and M refers to the ability of the patient to maintain alignment under binocular conditions. Orthoptic examination included evaluation of ocular movements and angle of strabismus. Angles of deviation were measured with the prism and alternate cover test for near (1/3 m) and distance fixation where possible. All children underwent evaluation with a slit lamp biomicroscope, cycloplegic refraction and dilated fundus examination with indirect ophthalmoscopy.
A detailed analysis of all the records, with respect to the ocular findings, systemic diagnoses, neuroimaging fi ndings and response to management modalities was done. All the children underwent a complete assessment, including medical history and ophthalmological and orthoptic examinations. An experienced pediatric ophthalmologist evaluated them and the neuroimaging studies, where available, were reviewed by a neuroradiologist. Visual acuity was recorded with the help of a Snellen’s chart and in cases where verbal visual acuity measurements were not possible due to age or associated systemic issues, the testing of visual response was done by monitoring the fixation in each eye by the Central, Steady, Maintained (CSM) method, where C refers to centrality and can be assessed by the location of the corneal light reflex as the patient looks at the examiner’s light with the opposite eye occluded, S refers to the steadiness of fixation on the examiner’s light under monocular conditions and M refers to the ability of the patient to maintain alignment under binocular conditions. Orthoptic examination included evaluation of ocular movements and angle of strabismus. Angles of deviation were measured with the prism and alternate cover test for near (1/3 m) and distance fixation where possible. All children underwent evaluation with a slit lamp biomicroscope, cycloplegic refraction and dilated fundus examination with indirect ophthalmoscopy.
Results
A total of 22 cases were identified. Of the 22, 15 (68.18%)
patients were male and seven (31.81%) were female. The
average age at presentation was 6.08 years (range, 4 months
to 16 years).
Only one patient (4.54%) had bilateral FNP and 21 cases (95.45%) had unilateral FNP.
The etiology of FNP in our series was variable. Seventeen patients (77.27%) had congenital palsy and of these, five patients had a syndromic association, three had birth trauma and nine patients had idiopathic palsy. Two patients were diagnosed to have Moebius syndrome, one each had Dandy Walker syndrome, oculoauriculovertebral malformation (Figure 1) and hemifacial microsomia (HFM).
Three patients had ipsilateral sixth nerve palsy, one underwent strabismus surgery for the resulting esotropia, both had amblyopia and required treatment. Two children were diagnosed to have Moebius syndrome and were treated conservatively. One child had an ipsilateral Duane’s syndrome with ipsilateral hearing loss (Figure 2). The Duane’s caused a mild face turn and patient did not require surgical management.
Corneal involvement was seen in eight patients (36.36%). Of these, three patients had superficial punctate erosions, two had a corneal opacity, three had exposure keratopathy, of which one developed a corneal ulcer and one was referred with a corneal perforation with vitreous prolapse. Six patients were treated conservatively with lubricants, two needed a lateral tarsorrhaphy and the patient with corneal perforation required a therapeutic penetrating keratoplasty with cataract extraction and anterior vitrectomy.
Another significant finding was that of amblyopia,
which was seen in ten patients (45.45%). Three patients
had strabismic amblyopia, three developed stimulation
deprivation amblyopia due to corneal opacity, two had
anisometropic amblyopia and two had a combination
of strabismic and anisometropic amblyopia. Amblyopia
therapy was done with optical correction and occlusion but
visual acuity improved in only three patients. Strabismus
surgery was done in two patients. Only one patient (4.54%) had bilateral FNP and 21 cases (95.45%) had unilateral FNP.
The etiology of FNP in our series was variable. Seventeen patients (77.27%) had congenital palsy and of these, five patients had a syndromic association, three had birth trauma and nine patients had idiopathic palsy. Two patients were diagnosed to have Moebius syndrome, one each had Dandy Walker syndrome, oculoauriculovertebral malformation (Figure 1) and hemifacial microsomia (HFM).

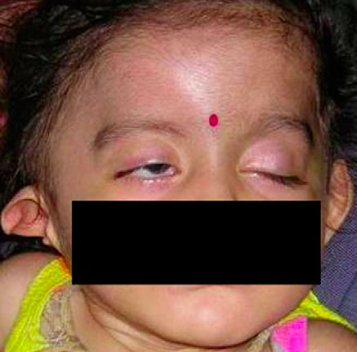
Figure 1 A child with right facial ner ve palsy (FNP) and
oculoauriculovertebral malformation with a deformed right pinna.
Five patients (22.72%) had an acquired palsy, of these,
two had a traumatic cause and one patient each had
neoplastic origin of the palsy, iatrogenic palsy after surgery
for hemangioma and idiopathic palsy.
The ocular findings included secondary effects of the
FNP as well as features related to various syndromes. Three patients had ipsilateral sixth nerve palsy, one underwent strabismus surgery for the resulting esotropia, both had amblyopia and required treatment. Two children were diagnosed to have Moebius syndrome and were treated conservatively. One child had an ipsilateral Duane’s syndrome with ipsilateral hearing loss (Figure 2). The Duane’s caused a mild face turn and patient did not require surgical management.

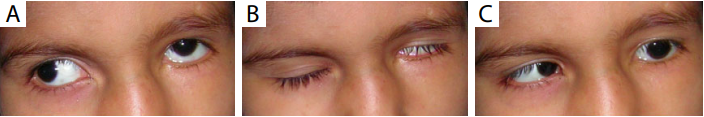
Figure 2 A children with facial nerve palsy (FNP) and ipsilateral Duane’s syndrome.
(A) Left eye—upshoot on adduction, limitation of
adduction; (B) left eye—lagophthalmos due to FNP; (C) left eye—limitation of abduction. Corneal involvement was seen in eight patients (36.36%). Of these, three patients had superficial punctate erosions, two had a corneal opacity, three had exposure keratopathy, of which one developed a corneal ulcer and one was referred with a corneal perforation with vitreous prolapse. Six patients were treated conservatively with lubricants, two needed a lateral tarsorrhaphy and the patient with corneal perforation required a therapeutic penetrating keratoplasty with cataract extraction and anterior vitrectomy.
The other systemic associations included cleft lip and palate, developmental delay and cerebral palsy.
Imaging studies were available in nine patients (40.90%). Of these, two patients had history of trauma with both the CT scans showing fracture of the occipital bone along with the petrous part of the temporal bone. One patient had an MRI scan showing a posterior fossa cyst and was diagnosed as Dandy Walker syndrome. In another patient, with ipsilateral sixth nerve palsy, MRI scan was suggestive of focal atrophic gliosis in the pons. Another patient, showed an intracranial lesion suggestive of a chloroma. One patient, with Moebius syndrome, showed a thinning of the lateral rectus muscle with absent parotid gland and temporalis muscle on computed tomography (CT) scan. One patient with HFM showed small middle ear cavity with ossicular chain deformity on CT scan. Two patients had normal imaging studies.
Discussion
Paralysis of the facial nerve can potentially affect vision, causes lack of facial expression and impacts social interaction(4).
A large proportion of pediatric facial nerve palsies are secondary in nature and thus prompt diagnosis and treatment is very important. Idiopathic FNP is the commonest cause of FNP in children(5,6). We found no identifiable cause in ten out of 22 children (45.4%). Birth trauma is quite common; with 78-90% of facial nerve palsies in the new born being attributed to birth trauma(3). We had three patients (13.63%) with birth trauma due to forceps delivery. Congenital FNP is associated with a number of syndromes including Moebius syndrome, CHARGE syndrome, Goldenhar syndrome, Di George syndrome and muscular dystrophy(7). In our study, five patients (22.72%) had a syndromic association, of these, two had Moebius syndrome, one had Dandy Walker syndrome, one had oculoauriculovertebral malformation, and one had HFM. HFM is a craniofacial disorder in which facial nerve dysfunction is common and has important implications in treatment(8). Acute otitis media and other infectious causes have been said to be very common causes of FNP in children(3,4), but our study did not show similar findings. This may be explained by the fact that our study was carried out at an ophthalmic center while previous studies were done in otolaryngology centers. We emphasize the need for a detailed systemic evaluation in all children presenting with FNP, to rule out any syndromic association or a potentially life threatening cause such as a neoplasm. Neuroimaging is a very useful tool in the evaluation and management of these children. In our study, neuroimaging results showed skull bone fractures in trauma, posterior fossa cyst, pontine gliosis and neoplasms. We recommend that all children presenting with FNP, congenital or acquired undergo neuroimaging. Corneal manifestations can range from superfi cial punctate erosions to severe exposure keratopathy with corneal perforation. Treatment must be initiated at the earliest. Mild keratopathy may be treated with lubricants, whereas severe exposure keratopathy may need surgical correction(9,10). These children are at risk for amblyopia due to a number of reasons. The corneal exposure may result in corneal opacities and predispose the child to stimulus deprivation amblyopia, the associated sixth nerve palsies result in strabismus and can result in amblyopia, also we found that four of the children in our series, had a component of anisometropia contributing to their amblyopia. Our study, thus, highlights the need for careful visual acuity testing and institution of prompt amblyopia therapy in these children.Conclusions
In summary, ophthalmologists must be aware of pediatric
FNP and its causes and complications. Any underlying
cause must be recognized and treated. The main priority
is to diagnose and treat corneal exposure, but in children,
amblyopia must be kept in mind. Appropriate referral to
oculoplastic surgeons and pediatricians is indicated as per
individual case requirements.
基金
暂无基金信息
参考文献
1. El-Hawrani AS, Eng CY, Ahmed SK, et al. General practitioners' referral pattern for children with acute facial paralysis. J Laryngol Otol 2005;119:540-2.
2. Grundfast KM, Guarisco JL, Thomsen JR, et al. Diverse etiologies of facial paralysis in children. Int J Pediatr Otorhinolaryngol 1990;19:223-39.
3. Shargorodsky J, Lin HW, Gopen Q. Facial nerve palsy in the pediatric population. Clin Pediatr (Phila) 2010;49:411-7.
4. Evans AK, Licameli G, Brietzke S, et al. Pediatric facial nerve paralysis: patients, management and outcomes. Int J Pediatr Otorhinolaryngol 2005;69:1521-8.
5. Cha HE, Baek MK, Yoon JH, et al. Clinical features and management of facial nerve paralysis in children: analysis of 24 cases. J Laryngol Otol 2010;124:402-6.
6. May M, Fria TJ, Blumenthal F, et al. Facial paralysis in children: diff erential diagnosis. Otolaryngol Head Neck Surg 1981;89:841-8.
7. Melvin TA, Limb CJ. Overview of facial paralysis: current concepts. Facial Plast Surg 2008;24:155-63.
8. Carvalho GJ, Song CS, Vargervik K, et al. Auditory and facial nerve dysfunction in patients with hemifacial microsomia. Arch Otolaryngol Head Neck Surg 1999;125:209-12.
9. Hazin R, Azizzadeh B, Bhatti MT. Medical and surgical management of facial nerve palsy. Curr Opin Ophthalmol 2009;20:440-50.
10. Lee V, Currie Z, Collin JR. Ophthalmic management of facial nerve palsy. Eye (Lond) 2004;18:1225-34.
相关文章
Jingyun Wang;Lyne Racette;Paxton Ott;Dana L. Donaldson;Daniel E. Neely; David A. Plager,Objectively-measured compliance to atropine penalization treatment in children with amblyopia: a pilot studySailaja Bondalapati;Avinash Pathengay;Jay Chhablani,External drainage for exudative retinal detachment secondary to central serous chorioretinopathyPrakash Paudel;Thomas Naduvilath;Vilas Kovai;Ha Thanh Phuong;Suit May Ho;David Wilson,Health literacy of adult Vietnamese population in relation to common eye conditions and factors for not seeking an eye examination