Integrating a flipped classroom and problem-based learning into ophthalmology education
阅读量:1363
DOI:doi: 10.3978/j.issn.1000-4432.2017.03.04
发布日期:2024-12-28
作者:
Jingyi Luo ,Tao Lin ,Nan Wang ,Yuxian Zou ,Xing Liu ,Chengguo Zu
展开更多 '%20fill='white'%20fill-opacity='0.01'/%3e%3cmask%20id='mask0_3477_29692'%20style='mask-type:luminance'%20maskUnits='userSpaceOnUse'%20x='0'%20y='0'%20width='16'%20height='16'%3e%3crect%20id='&%23232;&%23146;&%23153;&%23231;&%23137;&%23136;_2'%20x='16'%20width='16'%20height='16'%20transform='rotate(90%2016%200)'%20fill='white'/%3e%3c/mask%3e%3cg%20mask='url(%23mask0_3477_29692)'%3e%3cpath%20id='&%23232;&%23183;&%23175;&%23229;&%23190;&%23132;'%20d='M14%205L8%2011L2%205'%20stroke='%23333333'%20stroke-width='1.5'%20stroke-linecap='round'%20stroke-linejoin='round'/%3e%3c/g%3e%3c/g%3e%3c/svg%3e)
关键词
Flipped classroom (FC)
integrated
ophthalmology education
problem-based learning (FBL)
undergraduate
摘要
Background: Ophthalmology is an important medical science subject, but it is given with insufficient
attention in undergraduate medical education. Flipped classroom (FC) and problem-based learning (PBL)
are well-known education methods that can be integrated into ophthalmology education to improve students'
competence level and promote active learning.
Methods: We used a mixed teaching methodology that integrated a FC and PBL into a 1-week
ophthalmology clerkship for 72 fourth-year medical students. The course includes two major sessions: FC
session and PBL session, relying on clinical and real-patient cases. Written examinations were set up to assess
students’ academic performance and questionnaires were designed to evaluate their perceptions.
Results: The post-course examination results were higher than the pre-course results, and many students
gained ophthalmic knowledge and learning skills to varying levels. Comparison of pre- and post-course
questionnaires indicated that interests in ophthalmology increased and more students expressed desires to be
eye doctors. Most students were satisffed with the new method, while some suggested the process should be
slower and the communication with their teacher needed to strengthen.
Conclusions: FC and PBL are complementary methodologies. Utilizing the mixed teaching meth of FC
and PBL was successful in enhancing academic performance, student satisfactions and promoting active
learning.
全文
Introduction
Ophthalmology is an essential part of medical curriculum
system. Gaining medical knowledge of the eyes (e.g.,
ocular anatomy, red eye, common diseases of vision loss,
ophthalmic emergencies, relationships between eyes and
systemic diseases) and the skills of basic eye examinations
are critical for all medical students and physicians (1).
Unfortunately, in China, the quality of ophthalmology
education in undergraduates is relatively inadequate,
thus students do not acquire sufficient understanding of
eye diseases. This lack of knowledge may be attributed
to limited class time and lack of financial resources. As
ophthalmology is not a subject in post-graduate entrance
examinations or medical qualification examinations in
the China, many medical colleges do not emphasize
ophthalmology education, and students put less efforts into learning this subject. As a consequence, they are
inadequately trained to solve the most basic eye-related
problems, and majority of students do not acquire an
interest in pursuing a career in ophthalmology. Therefore,
a more active, self-directed learning approach needs to be
incorporated into the ophthalmology curricula.
Flipped classroom (FC) and problem-based learning
(PBL) are well-known active-learning pedagogical
strategies. Compared to traditional lecture, FC can promote
academic performance, student satisfaction, and active
learning (2-5). It is alleged that the FC model can facilitate
low-level learning (basic concepts) outside of class and highlevel
(application of knowledge) learning in-class. Students
can develop deeper understanding and higher-order
thinking throughout the process. Similarly, PBL is effective
in stimulating interests and promoting self-directed
learning (6). Implementation of PBL into medical courses
can also assist students in developing lifelong habits of
independent-learning, clinical reasoning, and collaboration (7-9). The FC contributes to setting up the framework for
conceptual knowledge, while PBL is a more interactive
methodology that helps to narrow the gap between theory
and practice.
We hypothesized that integrating a FC with PBL (FC&PBL), taking advantage of both approaches,
would be an effective method to improve undergraduate
students’ competence in ophthalmology and encourage
active learning. The intent of this study was to assess the
performance and perception of students by using both
approaches in ophthalmology clerkships and evaluating
whether their attitudes became more positive towards
ophthalmology after the clerkship.
(II) PBL session: students acquired the medical histories of patients with ocular blunt trauma in face-toface interactions. Related information such as visual acuity, intraocular pressure, and ocular findings were given to students in electronic form before the PBL. Teachers assigned homework consisting of “what auxiliary examinations should be taken”, “what is the probable diagnosis” and “select an appropriate treatment” for the provided case. The PBL process consisted of many steps (10). Pre-class, students worked in teams to clarify the patient’s situation, explain the possible causes of the signs and symptoms, list the necessary examinations and develop a preliminary diagnosis. In class, representatives of each team presented a slideshow of the group’s thoughts and diagnosis. Students from the other teams could raise concerns and put forward their own views. After that, teachers gave information of further examinations. Then students researched and integrated the new information into their diagnosis and treatment plans by synthesizing a comprehensive explanation and discussing the different opinions. Lastly, the teacher would systematically explain the patient’s diagnosis and treatment, summarizing the presentations and answering questions.
Students were encouraged to ask questions and make comments throughout the course. The teachers acted as guides facilitating the process. Students were also introduced to the basic skills of ocular examination including vision testing, slit-lamp examination and direct ophthalmoscopy to make them better understand the clinical features of eyes.
Methods
We used a mixed teaching method of integrating a FC and
PBL approaches as the basis for our study.
Subjects and setting
A total of 72 fourth-year undergraduates in the clinical
medicine specialty at Sun Yat-sen University were enrolled
in our study. Before starting this course, the students
completed the traditional ophthalmology theoretical course
and passed the final examination. The mixed-teachingmethod
course was administered in 1-week rotations
delivered to approximately 24 students per round. In every
rotation, students were divided into two cooperative teams
that consisted of several small groups with 4 to 5 students
and a teacher. Informed oral consent was obtained from
each student, teacher, and patient in this study. The quality
of every rotation was equivalent and the teachers were
experienced ophthalmologists from Zhongshan Ophthalmic
Center. Additionally, approval was received from the
Institutional Review Board of the Zhongshan Ophthalmic
Center (2017KYPJ025).
Study design
The course relied on clinical and real-patient cases that
varied from ocular anatomy to ocular trauma as well as
other common diseases of ophthalmology. Course design
was guided by a desire to make students better able to meet
the following learning objectives: (I) develop interests in
ophthalmology and better understand ophthalmology; (II)
improve ability to assess common eye diseases and manage
ophthalmic emergencies; and (III) cultivate students’
learning ability to better prepare for their future roles in
clinical work.
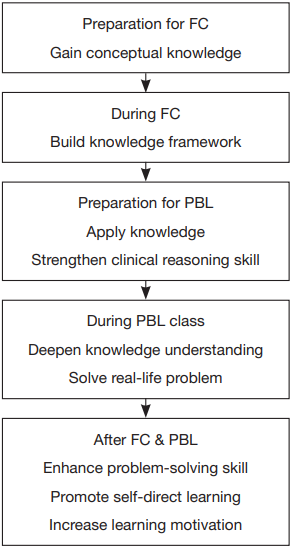
There are two major sessions in the course (Figure 1):
(I) FC session: students were provided with information,
instruction, and websites related to FC and PBL before the class. Online resources, including recorded
lectures, theoretical slides, operational videos and
chapter exercises, were provided to assist students’
learning. Students could utilize other websites,
professional books or the related literature to fill
gaps in the provided educational resources. During
class, students were asked to be the teacher and they
gave lectures on what they had learned. Each group
summed up what they had learned and then posed
questions. The next group was required to find the
answers and solve problems using what they had
learned. Group teachers gave feedback on these
problems, helped to answer questions, and corrected
mistakes. The preparation and implementation
of the FC provided students with a theoretical
ophthalmology base for the subsequent PBL; (II) PBL session: students acquired the medical histories of patients with ocular blunt trauma in face-toface interactions. Related information such as visual acuity, intraocular pressure, and ocular findings were given to students in electronic form before the PBL. Teachers assigned homework consisting of “what auxiliary examinations should be taken”, “what is the probable diagnosis” and “select an appropriate treatment” for the provided case. The PBL process consisted of many steps (10). Pre-class, students worked in teams to clarify the patient’s situation, explain the possible causes of the signs and symptoms, list the necessary examinations and develop a preliminary diagnosis. In class, representatives of each team presented a slideshow of the group’s thoughts and diagnosis. Students from the other teams could raise concerns and put forward their own views. After that, teachers gave information of further examinations. Then students researched and integrated the new information into their diagnosis and treatment plans by synthesizing a comprehensive explanation and discussing the different opinions. Lastly, the teacher would systematically explain the patient’s diagnosis and treatment, summarizing the presentations and answering questions.
Students were encouraged to ask questions and make comments throughout the course. The teachers acted as guides facilitating the process. Students were also introduced to the basic skills of ocular examination including vision testing, slit-lamp examination and direct ophthalmoscopy to make them better understand the clinical features of eyes.

Figure 1 Learning process of and problem-based learning (FC
& PBL).
Measures of effect
A written examination paper was set up to evaluate students’
academic performance. The theoretical examination is
the pre-course exam and the written examination after
the clerkship is the post-course exam. Both the pre-course
and the post-course exams were consistent in format and
knowledge range of ophthalmic diseases. The knowledge
range contained ocular trauma, keratonosus, glaucoma,
cataract and uveitis. The post-course exam contained casebased
problems, which further assessed the students’ clinical
analysis and knowledge application abilities. Post-course
scores were compared with pre-course scores to objectively
evaluate the teaching effect.
Measures of affect
The pre-course questionnaire contained nine statements
and post-course questionnaire contained 30 statements
that evaluated students’ perception of the course. Each
statement of the questionnaire used a 4-point Likert scale,
ranging from 1 (strongly disagree) to 4 (strongly agree)
(Figure 2). The post-course questionnaire repeated the nine
statements of pre-course questionnaire and added 21 extra
questions to understand the students’ experiences in the
ophthalmology clerkship. Additionally, students could write
down their feelings and suggestions at the end of the survey,
and the responses were categorized into groups. Precourse
questionnaires and post-course questionnaires were
completed by students at the beginning of the course and at
the end of the course, respectively. The difffculties of preand
post-course questionnaires are similar.
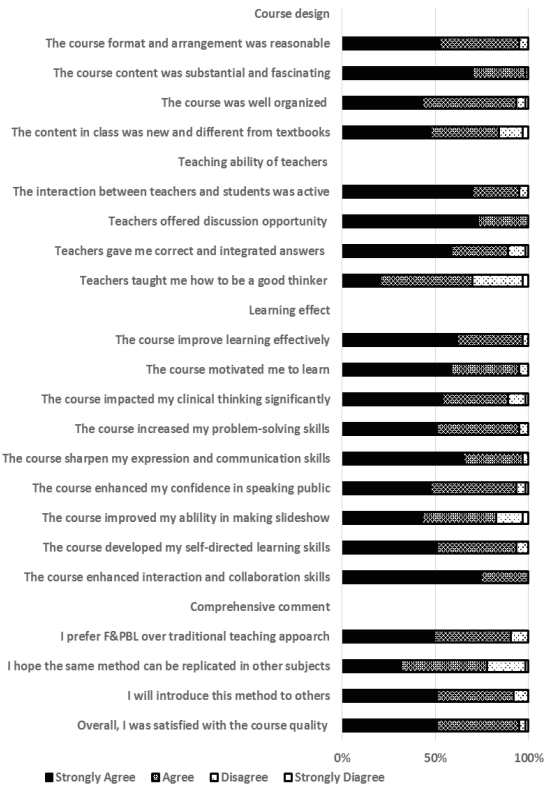

Figure 2 The additional 21 questions of post-course questionnaire.
Data analysis
Paired t-test was used to analyse pre-course and postcourse
examination results. After collapsing the responses
of the nine identical statements into two categories: agree
(indicates “strongly agree” and “agree”) and disagree
(represents “disagree” and “strongly disagree”), the
comparison of pre- and post-course results were analysed
using exact McNemar’s test. All analyses were output by
SPSS for windows version 22.0 (IBM, Armonk, NY, USA).
A P value less than 0.05 was considered significant.
Results
There were 72 fourth-year medical undergraduates that
participated in this study. Sixty-three students (87.5% response
rate) completed all the examinations and questionnaires. The
reason of loss to follow-up might be that some students failed
to hand in the examination papers or questionnaires and some
students were absent of the class. The result analysis excluded
the loss to follow-up participants.
Academic performance of pre- and post-course examinations
Examination results of all the students from the theoretical
course and the clerkship were collected and analysed. Postcourse
results (range from 60 to 93.5; mean score 86.3000;
standard deviation 5.8146) were significantly higher than
pre-course results (range from 72 to 100; mean score
79.0079; standard deviation 7.5169) (mean increase of 7.29;
95% confidence interval, 5.18-9.41; P<0.0001) (Figure 3).
The gap between high scores and low scores was narrow.
Forty-nine students (77.78%) gained ophthalmic knowledge
and learned skills to different degrees (10.59±6.20).
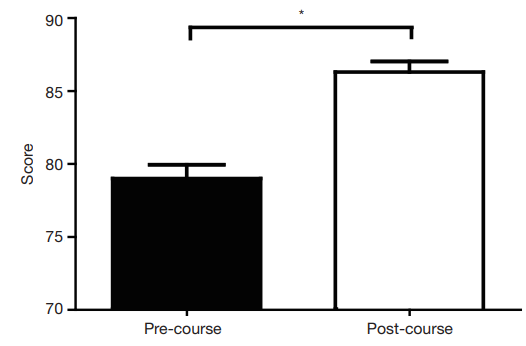

Figure 3 Comparison of pre- and post-course written examination
results. *, statistical signiffcance.
Student perception
The statements on the pre-course questionnaire were
designed to establish a baseline of the students’ attitudes
and preferences before class (Table 1). The majority of
students were willing to participate in FC & PBL and
quite optimistic about learning ophthalmology before
class. Thirty-nine (61.90%) students agreed and strongly
agreed that they had motivation to study ophthalmology
throughout their life, but only 5 (7.94%) students wanted
to be ophthalmologists. Responses to questions 7 through 9
indicated that a certain number of students felt stressful and
reluctant to do the presentations and were afraid that the
implementation of FC & PBL would disturb their daily life.
Comparison of pre-and post-course questionnaires indicated remarkable changes in four questions. After class, the interest and motivation to study ophthalmology increased, and 24 (38.10%)students expressed desires to be eye doctors, which is significantly higher than pre-course responses. Additionally, the number of students that felt stressful about the class reduced.
The 21 additional post-course questions were set up
to have a deeper insight into the influence of FC & PBL
on the learning experience, including course design, the
teaching ability of the teachers, the learning effect and
comprehensive comments (Figure 2). All of the statements
received more than 50% positive responses. Most of the
students were satisffed with the course design and teachers’
teaching abilities.
For the learning effect perception, students strongly agreed or agreed that the course improved learning knowledge effectively (n=61, 96.83%), motivated students to learn (n=60, 95.24%), impacted clinical thinking signiffcantly (n=56, 88.89%) and increased problem-solving skills (n=60, 95.24%). Of the 63 respondents, 57 (90.48%) participants preferred the FC & PBL model over the traditional course format, and 95.24% were satisfied with the quality of the course. All students strongly agreed or agreed that teachers offered opportunities for discussion and the course enhanced interaction and collaboration skills immensely. However, perceptions on “teachers taught me how to be a good thinker” and “I hope the same method can be replicated in other subjects” had relatively less positive responses, but the number of strongly agree and agree still accounted for more than half of respondents.
In the open-ended section for suggestions and feelings, majority of students considered the new method in ophthalmology clerkship fresh and attractive. Students spent a lot more time preparing than in the traditional class, but the rewards were greater. Whereas some students argued that they were incapable of finding satisfying answers. A part of students suggested that the process could be slower so that they could grasp the core concepts more clearly. Another suggestion was that more communication with teachers was needed outside of the classroom.
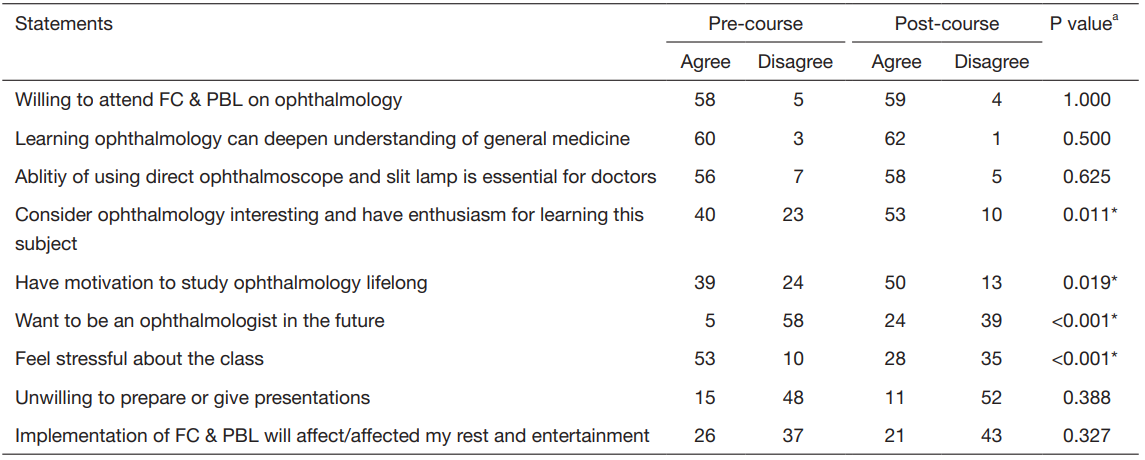 a , exact McNemar’s test;
*,
statistical significance; FC & PBL, flipped classroom and problem-based learning.
a , exact McNemar’s test;
*,
statistical significance; FC & PBL, flipped classroom and problem-based learning.
Comparison of pre-and post-course questionnaires indicated remarkable changes in four questions. After class, the interest and motivation to study ophthalmology increased, and 24 (38.10%)students expressed desires to be eye doctors, which is significantly higher than pre-course responses. Additionally, the number of students that felt stressful about the class reduced.
For the learning effect perception, students strongly agreed or agreed that the course improved learning knowledge effectively (n=61, 96.83%), motivated students to learn (n=60, 95.24%), impacted clinical thinking signiffcantly (n=56, 88.89%) and increased problem-solving skills (n=60, 95.24%). Of the 63 respondents, 57 (90.48%) participants preferred the FC & PBL model over the traditional course format, and 95.24% were satisfied with the quality of the course. All students strongly agreed or agreed that teachers offered opportunities for discussion and the course enhanced interaction and collaboration skills immensely. However, perceptions on “teachers taught me how to be a good thinker” and “I hope the same method can be replicated in other subjects” had relatively less positive responses, but the number of strongly agree and agree still accounted for more than half of respondents.
In the open-ended section for suggestions and feelings, majority of students considered the new method in ophthalmology clerkship fresh and attractive. Students spent a lot more time preparing than in the traditional class, but the rewards were greater. Whereas some students argued that they were incapable of finding satisfying answers. A part of students suggested that the process could be slower so that they could grasp the core concepts more clearly. Another suggestion was that more communication with teachers was needed outside of the classroom.
Table 1 Comparison of pre-course and post-course perception on FC & PBL (n=63)

Discussion
The results of current study show that utilizing FC and PBL
increased students’ knowledge and produce more positive
attitudes towards ophthalmology. We were delighted to
see that the number of students that now aspire to be eye
doctors markedly increased after the clerkship.
The advantages of FC and PBL have been revealed in
this study. The post-course examination contained casebased
problems, and the improved results demonstrated the
students’ comprehension of clinical analysis and knowledge application. Although most students were satisfied with
this study, some students were not. Some students did not
understand the class well and had low efficiency in their
searches for satisfactory answers, which might due to their
unfamiliarity with active learning modules. Some of them
wished to have communication with teachers. Hence, it is
necessary to promote active learning methods in medical
education and teachers have to put more effort into
interactions with students.
Ophthalmology is a relatively underrepresented medical specialty. As such, little effort has been put into the curriculum by educational institutions and students. Combined with traditional didactic teaching models, students’ passion for learning ophthalmology is relatively nonexistent. Both FC and PBL are feasible ways to reverse the declining trend of ophthalmology education (5,8,11,12). In FC, students study independently to gain conceptual knowledge. In-class teaching is based on teacher-student interactions instead of one-way lecturing, which leads to greater student engagement, enhanced motivation to learn, more positive attitudes, and better relationships between teachers and students (13). PBL is another active learning approach. Preparation for PBL is a process of applying knowledge and strengthening clinical reasoning skills. In this manner, students learn about a subject by exploring an unstructured topic. Moreover, it emphasizes the application of theoretical knowledge to solve problems in the real world. Students are allowed to stage a debate during the class, where they have to articulate their thoughts and develop arguments to support their views. Communication, problem-solving, and critical-thinking skills are fostered in the process.
Nevertheless, some educators argue that PBL is not better than traditional teaching methodologies in improving learning outcomes. This may be due to student unfamiliarity with the new module or inadequate understanding of basic concepts (14,15). Adopting a FC to facilitate conceptual framework formation is an optimal solution for this problem. Until now, educators understood that integrating a FC and PBL was a possibility, but few studies document the combination. These two methodologies share an emphasis on higher order thinking skills, and are used in conjunction with one another. That is, they are complementary. Using FC&PBL maximizes class time and allows students to learn individually or through group activities. Without PBL, students put less effort into understanding concepts, and they do not learn how to handle real life problems. Likewise, implementing PBL without FC module will require too much class time for teaching and learning to be able to apply the knowledge. The FC provides a promising framework of knowledge for PBL instruction, which promotes information retention.
Meanwhile, because ophthalmology is a visual science and ophthalmologists make judgements on visual characteristics, we applied clinical cases, real patients, and slit-lamp multimedia systems as subsidiary strategies to improve class quality (16). Besides, we used ocular trauma as the major content of case discussions. Ocular trauma is an ophthalmic emergency that needs considerable attention. It is a preferable discussion topic due to its complexity and various clinical features. Clinical images of ocular traumas are available to show different signs, so students can see exactly what the clinical features look like. Multimedia systems can assist teachers in demonstrating the dynamic changes from real patients, such as iridodonesis.
There were several limitations in our study. First, the PBL team size was large, thus few students had frequent chances to make statements or communicate with others. Second, because the teaching faculty had to pay attention to everyone’s performance, not receiving enough individual attention may have negatively affected some students’ attitudes. Third, as the participants were voluntarily taking part in our study, the willingness of active learning might influence the teaching outcome and we cannot evaluate the effect among the less initiative students. Fourth, there was not a control group to compare the effectiveness of the format, due to ethical problems and time constraints. Further studies and investigations are required that include a control group to obtain a better understanding of this methodology. Additionally, it might take a lot of time for students to prepare the class, and further and more extensive studies would find out the practicality of these approaches. Another limitation was that some sections like diabetic retinopathy and age-related macular degeneration were not included in our study, and we will add these sections in the future study.
Ophthalmology is a relatively underrepresented medical specialty. As such, little effort has been put into the curriculum by educational institutions and students. Combined with traditional didactic teaching models, students’ passion for learning ophthalmology is relatively nonexistent. Both FC and PBL are feasible ways to reverse the declining trend of ophthalmology education (5,8,11,12). In FC, students study independently to gain conceptual knowledge. In-class teaching is based on teacher-student interactions instead of one-way lecturing, which leads to greater student engagement, enhanced motivation to learn, more positive attitudes, and better relationships between teachers and students (13). PBL is another active learning approach. Preparation for PBL is a process of applying knowledge and strengthening clinical reasoning skills. In this manner, students learn about a subject by exploring an unstructured topic. Moreover, it emphasizes the application of theoretical knowledge to solve problems in the real world. Students are allowed to stage a debate during the class, where they have to articulate their thoughts and develop arguments to support their views. Communication, problem-solving, and critical-thinking skills are fostered in the process.
Nevertheless, some educators argue that PBL is not better than traditional teaching methodologies in improving learning outcomes. This may be due to student unfamiliarity with the new module or inadequate understanding of basic concepts (14,15). Adopting a FC to facilitate conceptual framework formation is an optimal solution for this problem. Until now, educators understood that integrating a FC and PBL was a possibility, but few studies document the combination. These two methodologies share an emphasis on higher order thinking skills, and are used in conjunction with one another. That is, they are complementary. Using FC&PBL maximizes class time and allows students to learn individually or through group activities. Without PBL, students put less effort into understanding concepts, and they do not learn how to handle real life problems. Likewise, implementing PBL without FC module will require too much class time for teaching and learning to be able to apply the knowledge. The FC provides a promising framework of knowledge for PBL instruction, which promotes information retention.
Meanwhile, because ophthalmology is a visual science and ophthalmologists make judgements on visual characteristics, we applied clinical cases, real patients, and slit-lamp multimedia systems as subsidiary strategies to improve class quality (16). Besides, we used ocular trauma as the major content of case discussions. Ocular trauma is an ophthalmic emergency that needs considerable attention. It is a preferable discussion topic due to its complexity and various clinical features. Clinical images of ocular traumas are available to show different signs, so students can see exactly what the clinical features look like. Multimedia systems can assist teachers in demonstrating the dynamic changes from real patients, such as iridodonesis.
There were several limitations in our study. First, the PBL team size was large, thus few students had frequent chances to make statements or communicate with others. Second, because the teaching faculty had to pay attention to everyone’s performance, not receiving enough individual attention may have negatively affected some students’ attitudes. Third, as the participants were voluntarily taking part in our study, the willingness of active learning might influence the teaching outcome and we cannot evaluate the effect among the less initiative students. Fourth, there was not a control group to compare the effectiveness of the format, due to ethical problems and time constraints. Further studies and investigations are required that include a control group to obtain a better understanding of this methodology. Additionally, it might take a lot of time for students to prepare the class, and further and more extensive studies would find out the practicality of these approaches. Another limitation was that some sections like diabetic retinopathy and age-related macular degeneration were not included in our study, and we will add these sections in the future study.
Conclusions
The study is a preliminary attempt to integrate the FC
and PBL approaches in ophthalmology education. This
relatively cost-effective methodology provides an engaging
and active learning environment where students can gain
ophthalmic knowledge, clinical skills, problem-solving
abilities, self-directed learning abilities, and motivations.
All of these elements contribute to the lifelong professional
growth of medical students and can assist in their future
careers.
基金
1. This work was supported by National Natural
Science Foundation of China for Young Scientist (81200686,
81400426), Research Fund for the Doctoral Program of
Higher Education of China (20120171120108), Natural
Science Foundation of Guangdong Province, China
(S2011040005378), Fundamental Research Funds for the
Central Universities (11ykpy65, 15ykpy31).
参考文献
1. Clarkson JG. Training in ophthalmology is critical for all physicians. Arch ophthalmol 2003;121:1327.
2. Gillispie V. Using the Flipped Classroom to Bridge the Gap to Generation Y. Ochsner J 2016;16:32-6.
3. Khanova J, McLaughlin JE, Rhoney DH, et al. Student Perceptions of a Flipped Pharmacotherapy Course. Am J Pharm Educ 2015;79:140.
4. Missildine K, Fountain R, Summers L, et al. Flipping the classroom to improve student performance and satisfaction. J Nurs Educ 2013;52:597-9.
5. Wakabayashi N. Flipped classroom as a strategy to enhance active learning. Kokubyo Gakkai Zasshi. 2015;81-82:1-7.
6. Al Wadani F, Khan AR. Problem-based learning in ophthalmology: A brief review. Oman J Ophthalmol 2014;7:1-2.
7. Kaliyadan F, Amri M, Dhuffri M, et al. Effectiveness of a modiffed tutorless problem-based learning method in dermatology - a pilot study. J Eur Acad Dermatol Venereol 2012;26:111-3.
8. Kong J, Li X, Wang Y, et al. Effect of digital problembased learning cases on student learning outcomes in ophthalmology courses. Arch Ophthalmol 2009;127:1211-4.
9. Roberts C, Lawson M, Newble D, et al. The introduction of large class problem-based learning into an undergraduate medical curriculum: an evaluation. Med Teach 2005;27:527-33.
10. Schmidt HG. Problem-based learning: rationale and description. Med Educ 1983;17:11-6.
11. Farrell TA, Albanese MA, Pomrehn PR Jr. Problem-based learning in ophthalmology: a pilot program for curricular renewal. Arch Ophthalmol. 1999;117:1223-6.
12. Michael J. Where's the evidence that active learning works? Adv Physiol Educ 2006;30:159-67.
13. McLaughlin JE, Roth MT, Glatt DM, et al. The ffipped classroom: a course redesign to foster learning and engagement in a health professions school. Acad Med 2014;89:236-43.
14. Antepohl W, Herzig S. Problem-based learning versus lecture-based learning in a course of basic pharmacology: a controlled, randomized study. Med Educ 1999;33:106-13.
15. Li J, Li QL, Li J, et al. Comparison of three problembased learning conditions (real patients, digital and paper) with lecture-based learning in a dermatology course: a prospective randomized study from China. Med Teach 2013;35:e963-70.
16. Dammers J, Spencer J, Thomas M. Using real patients in problem-based learning: students' comments on the value of using real, as opposed to paper cases, in a problembased learning module in general practice. Med Educ 2001;35:27-34.
相关文章
罗明杰;张玮星;张哲铭;庞健宇;林桢哲;赵兰琴;林铎儒;林浩添,Harnessing AI–human synergy for deep learning research analysis in ophthalmology with large language models assisting humans陈灿;谢曜爵;翁一翠;王建;符飞芳;陈健辉;张晓晓,A machine-learning-based bibliometric analysis of the scientific literatures on orthokeratologyOwusu Gideon;Kyei Samuel;Sa-Ambo Joseph Mannyeya;Asiamah Randy;Owusu Paul;Agyiri Patrick Evans;Boadi-Kusi Samuel Bert;Amoako Pious Tawiah;Owusu Gideon,Bibliometric analysis of ophthalmology training institutions, distribution and sub-specializations in Africa